View Providers
Pacemaker Information You May Not Know
Pacemakers to treat hearts that beat too slowly (bradycardia) were invented in the 1950s, but it was only in 1969 when they were powered with lithium batteries that they became a viable treatment. Now, there are an estimated 200,000 pacemakers implanted each year in the United States to help patients with bradycardia. While technology has changed, allowing pacemakers to last longer and cause fewer complications, not everyone knows the latest pacemaker information or what happens with pacemaker insertion. Here are some facts about living with a pacemaker, including possible side effects.

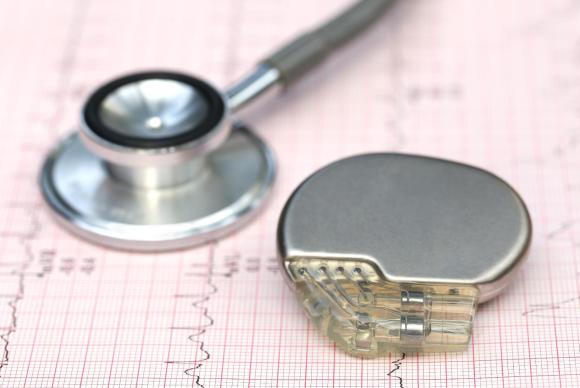
1. A pacemaker can fit in the palm of your hand.
It’s made of two parts: a generator, which is the device itself, and one or more wires connected to the pacemaker. The generator contains electric circuits and a battery. These wires, also called leads, sit directly in your heart so they can monitor your heart’s rhythms. The electrodes on the wires allow your pacemaker to detect the heartbeat and, if necessary, deliver an electrical current directly to your heart to stimulate a heartbeat.
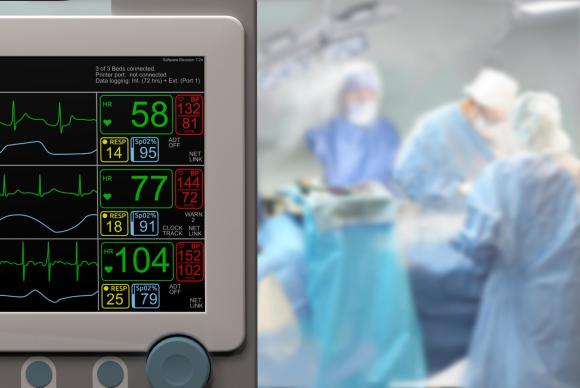
2. Insertion of a pacemaker is a minor surgical procedure.
For most people, a pacemaker insertion is a minor surgical procedure done with local anesthetic. A small incision, usually under the collarbone, allows your doctor to slip the pacemaker is just under the skin. It is then attached to a wire or wires that have been threaded through your vein leading directly to your heart. Once the pacemaker is in place, it’s tested to ensure it works before your doctor closes the incision. Although the pacemaker is technically “on” all the time, it only fires impulses when it detects your heartbeat has gone below a preset number of beats per minute.

3. Full recovery can take up to eight weeks.
After your procedure, your doctor will tell you about any restrictions or precautions you should take during the healing period, such as keeping the incision area dry, avoiding heavy lifting, or raising your arm above your head. Living with a pacemaker means being able to do things you wish you could do, such as being physically active, traveling, working or even having sexual relations. Because every patient is different, speak openly with your doctor about what you can and shouldn’t do during your recovery time.

4. There are few side effects related to a pacemaker.
There are few downsides or side effects related to having a pacemaker. You may experience pain or soreness for a while after the pacemaker insertion, but other than the initial healing time, you shouldn’t feel the device at all. However, even minor surgery carries a certain level of risk, such as infection, blood clots, bleeding at the incision, or swelling and bruising. Damage to the blood vessels by the wires as they are threaded to your heart is also a possibility. Your doctor may warn against you participating in contact sports, which may cause a blow to your chest area. To reduce your risk of procedure complications, the doctor performing your procedure should have a lot of experience and a low rate of complications. Ask your doctor to share this information with you.

5. You can travel with a pacemaker.
Having a pacemaker shouldn’t restrict your travel plans, even if you are flying. Before going through security, let the screening agents know about your pacemaker. You can request a manual screening with a hand wand. The walk-through screening device will not affect your pacemaker, but the metal in your device will likely be detected. You should always carry your pacemaker ID card (provided by the device manufacturer in case of emergency), especially while traveling. This card indicates the type of pacemaker you have, the number of leads, and your doctor’s name.

6. Pacemakers can be checked by phone.
After your pacemaker insertion, you will have a follow-up appointment so your doctor can check the incision and placement of your pacemaker. After the checkup, your pacemaker can be monitored by phone. A programming device over the pacemaker area sends signals over the phone line. Some newer pacemakers have remote heart monitoring with smart phone apps or over broadband frequencies. You will still need to see your doctor for regular checkups, but with remote monitoring your doctor makes sure your pacemaker is working correctly between office visits.
7. You will need a replacement pacemaker when the battery runs out.
How long your pacemaker battery lasts depends on how often the device sends electrical stimulation to your heart. The less frequently it does this, the longer your battery lasts. When your pacemaker needs a new battery, your doctor removes the pacemaker and inserts a new pacemaker generator. The wires generally stay in place unless they break or malfunction. As with insertion, the replacement is a minor surgical procedure.

8. Most everyday electronic devices will not affect your pacemaker.
Newer pacemakers are designed so most everyday electronic devices have no effect on them. This includes most home devices, such as electric shavers, heating pads, microwave ovens, TV remote controls, and more. It is generally safe to use a cell phone, but device manufacturers recommend you do not keep your cell phone near your chest. There is some concern that other devices, such as MRI (magnetic resonance imaging) machines, radiation machines for treating cancer, some dental equipment, power-generating equipment, and heavy equipment that contain magnets can affect how well your pacemaker works. Contact the pacemaker’s manufacturer if you have any concerns or questions about your pacemaker.
9. New leadless pacemakers don’t need a pocket to hold them.
A new type of pacemaker—one that doesn’t have wires or leads—was recently approved for people with certain types of bradycardia. The device is smaller than the traditional pacemaker and fits into the heart’s right ventricle, where it will emit a pulse when necessary. Currently, leadless pacemakers are for patients who only need the pacemaker to stimulate one chamber of the heart. They are not for people who have cardioverter defibrillators or certain types of heart malformations or heart disease.






